Carpal tunnel release surgery relieves nerve pressure but carries risks, recovery time, and mixed outcomes—making non-surgical treatments worth considering first.
Carpal tunnel release surgery is often presented as a definitive solution for persistent hand pain, numbness, and tingling caused by carpal tunnel syndrome. By cutting the ligament that compresses the median nerve, the procedure aims to reduce pressure and restore normal function. But while surgery can be effective in some cases, it’s far from a guaranteed fix.
In reality, outcomes vary widely. Some patients experience meaningful relief, while others continue to struggle with symptoms—or even develop new complications. Add to that the recovery time, potential risks, and lifestyle disruptions, and it becomes clear why most doctors recommend surgery only as a last resort.
This article breaks down everything you need to know about carpal tunnel release surgery—including who it’s best suited for, how it works, and the real pros and cons. Most importantly, it helps you understand whether surgery is truly necessary—or if safer, non-surgical options may offer better results with fewer risks.
Carpal tunnel release surgery is a procedure that reduces pressure on the median nerve by cutting the transverse carpal ligament. It can relieve symptoms like pain, numbness, and tingling, but results vary. Some patients experience full relief, while others have only partial improvement, persistent symptoms, or recurrence over time. Because of the risks, recovery time, and mixed satisfaction rates, surgery is typically recommended only after non-surgical treatments have failed.
Table of Contents
- Who Needs Carpal Tunnel Release Surgery?
- Carpal Tunnel Release Surgery: Pros and Cons
- When is Surgery Recommended?
- What Does the Surgery Involve?
- Pros of Carpal Tunnel Release Surgery
- Cons of Carpal Tunnel Release Surgery
- Recovery and Aftercare
- Potential Risks and Complications
- How Effective is Carpal Tunnel Surgery?
- Non-Surgical Alternatives
- Key Takeaways
FAQs
About
1. Who Needs Carpal Tunnel Release Surgery?
Carpal tunnel syndrome is a progressive condition that often worsens without treatment, which is why early intervention is important. However, surgery is not ideal for every patient—and outcomes can vary significantly.
Doctors caution that certain individuals may have a higher risk of poor surgical results. These risk factors include:
- Severe or advanced or very
severe carpal tunnel symptoms
- Age over 50
- Underlying health conditions such as diabetes, obesity, high blood pressure, or arthritis
- Lifestyle and behavioral factors like smoking, alcohol use, depression, or chronic stress
These factors can increase the likelihood that surgery will not fully relieve symptoms—or may fail altogether.
For this reason, it’s essential to have a detailed discussion with your doctor before considering surgery. Carpal tunnel release has both advantages and disadvantages, and should always be weighed carefully against effective non-surgical treatment options.
2. Carpal Tunnel Release Surgery: Pros and Cons
Carpal tunnel syndrome is a progressive condition that often worsens without treatment. While surgery can be effective in some cases, most doctors recommend it only after all non-surgical treatments have failed. Before deciding, it’s important to fully understand both the benefits and drawbacks.
3. When is Surgery Recommended?
Doctors typically recommend carpal tunnel release surgery only if all of the following apply:
- Non-surgical treatments have been tried for at least 6 months
- Symptoms remain
severe and interfere with daily life
- Conservative treatments have failed to provide relief
According to clinical guidance, non-surgical treatments are highly effective in many cases—so surgery is reserved for more advanced conditions.
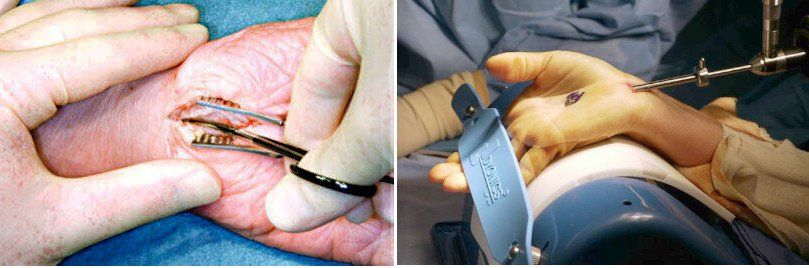
4. What Does the Surgery Involve?
Carpal tunnel surgery is usually performed on an outpatient basis using either local or
general anesthesia. There are two main types:
Endoscopic Release
(see more)
- Small incision(s) with a camera-guided tool
- Less tissue damage
- Faster
recovery and smaller scar
Open Release
(see more)
- Larger incision in the palm (2–3 inches)
- Better visibility for the surgeon
- Lower risk of accidental injury to nerves or vessels
The goal of each procedure is to locate and cut the
transverse carpal ligament. This holds the wrist bones together. The surgeon cuts the ligament which allows the bones snap apart. When that happens, it relieves pressure on the
median nerve beneath.
Your doctor will prefer one procedure over the other. Discuss this with your doctor
well before the surgery date. Discuss the pros and cons, how they impact your aftercare, and what they mean to your recovery time.
5. Pros of Carpal Tunnel Release Surgery
Endoscopic Surgery Advantages
- Less hand trauma
- Faster recovery time
- Smaller scar
Open Surgery Advantages
- Better visibility during surgery
- Lower risk of accidental nerve or vessel damage
- More widely performed by surgeons
Post-surgical results can vary widely. In many cases, symptoms improve within days, but for others, relief may take weeks or months. Some patients experience only partial improvement—or no improvement at all. In certain cases, symptoms may return after initially disappearing, and a small number of patients may even experience worsening symptoms after surgery.
6. Cons of Carpal Tunnel Release Surgery
Endoscopic Surgery Risks
- Limited visibility inside the wrist
- Higher risk of accidental injury
- More expensive and less widely available
Open Surgery Risks
- Larger incision and more tissue damage
- Longer recovery time
- Greater post-surgical pain
- More noticeable scar
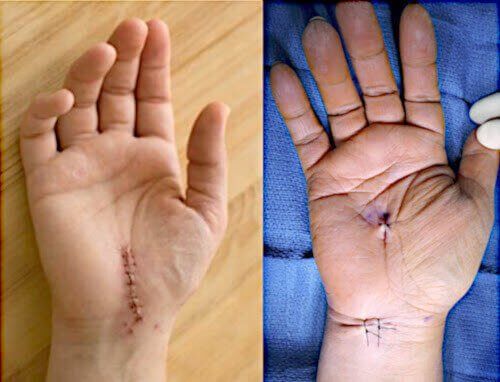
7. Recovery and Aftercare
Recovery depends on several factors:
- Endoscopic surgery: weeks to a few months
- Open surgery: often 2–3× longer recovery
Additional factors affecting recovery:
- Dominant vs. non-dominant hand
- Type of work (manual vs. sedentary)
- Commitment to hand therapy
Patients with physically demanding
jobs may require 3–6 months before returning to full activity. Note that only
10%of workers return their former jobs after carpal tunnel surgery.
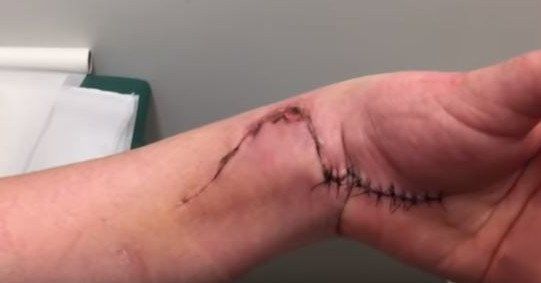
8. Potential Risks and Complications
Like all surgeries, carpal tunnel release carries risks, including:
- Persistent or recurring symptoms
- Nerve or blood vessel damage
- Loss of grip strength (sometimes permanent)
- Infection or scar tissue complications
- Ongoing post-surgical pain
In some cases, patients may require
additional (revision) surgery.
9. How Effective is Carpal Tunnel Surgery?
Success rates vary widely. While some doctors report a 10–15% failure rate, patient satisfaction tells a different story.
- About
50% of patients are satisfied after 2 years
- Others report partial relief—or no improvement at all
- Symptoms may return over time
This variability makes it essential to weigh surgery carefully against other options.
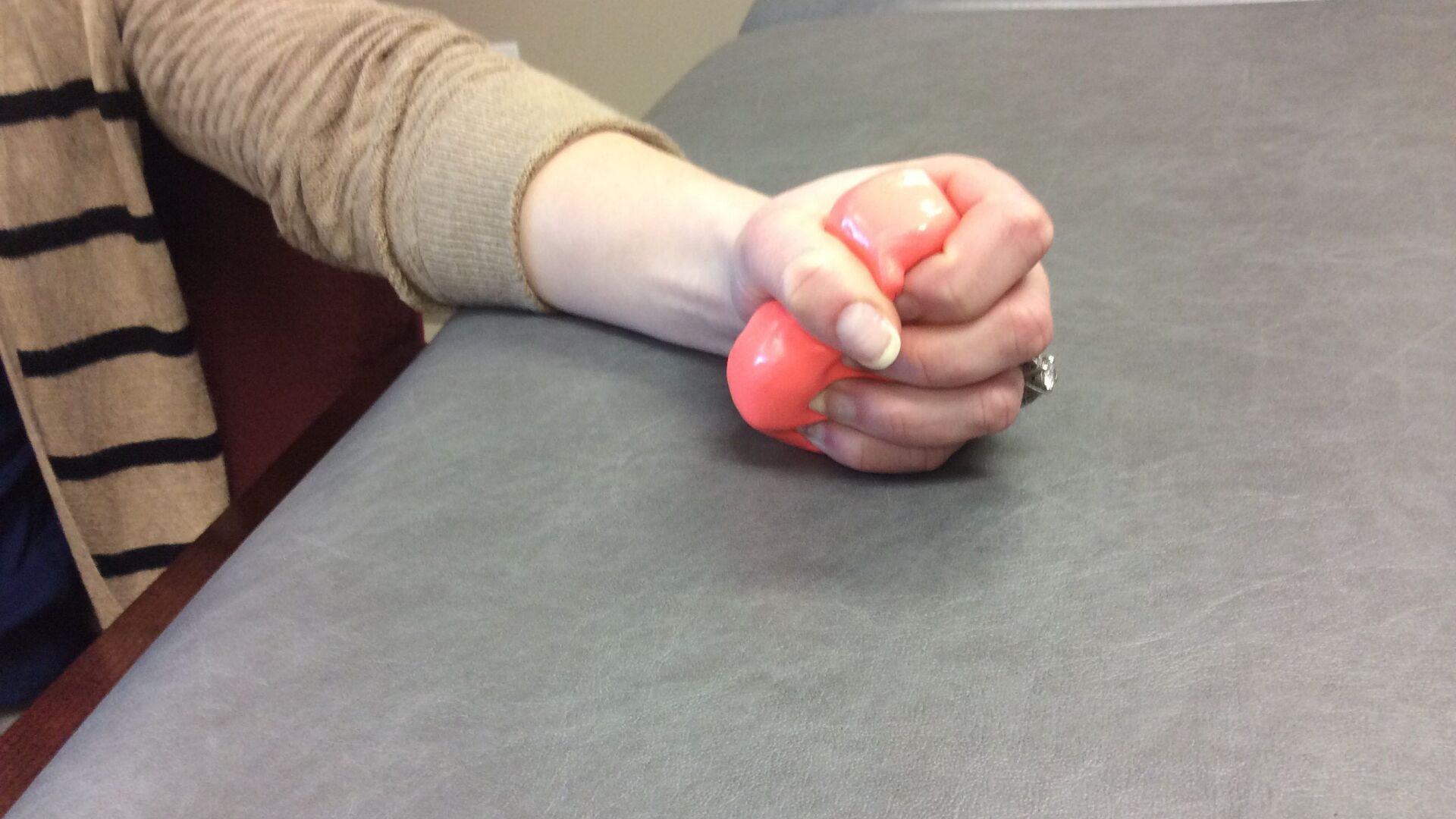
10. Non-Surgical Alternatives
Today, many patients successfully treat carpal tunnel syndrome without surgery. Proven
non-surgical optiions include:
- Night bracing
- Stretching exercises
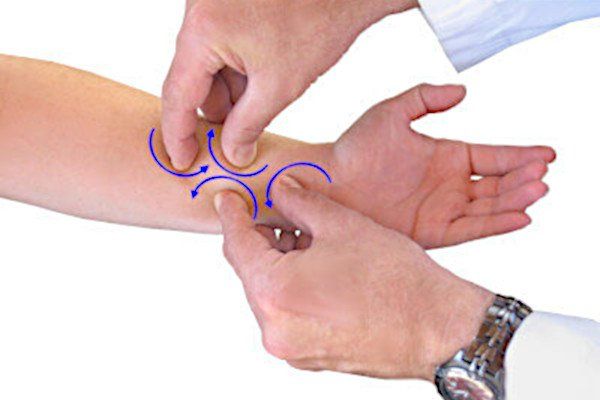
- Myofascial release therapy
These methods can be effective in over 90% of cases and often resolve symptoms faster than surgical recovery.
11. Key Takeaways
Carpal tunnel release surgery can provide relief—but it’s not always the best first option. With real risks, recovery time, and mixed satisfaction rates, it’s critical to explore non-surgical treatments first and carefully weigh all pros and cons with your doctor.
Frequently Asked Questions
How successful is carpal tunnel release surgery?
Success varies. Some patients get complete relief, while others continue to have symptoms or see them return over time.
How long does it take to recover from carpal tunnel surgery?
Recovery may take a few weeks to several months, depending on the type of surgery and how much you use your hand.
Should I try non-surgical treatments before surgery?
Yes. Most doctors recommend trying bracing, stretching, and other non-surgical treatments first because they are often effective.
About Dr. Z